(May 2, 2019) The Alabama Medicaid Program imposes significant exclusion screening requirements on its providers. Many are unaware of the extent of their exclusion screening obligations or of the severe consequences that can result from a failure to properly screen. This short summary has been prepared to help further provider awareness of the exclusion screening rules and regulations in force and the effect of an Alabama exclusion.
I. Basic Alabama Exclusion Screening Requirements
Providers must screen all employees and contractors by searching the Alabama Medicaid Exclusion List, the HHS-OIG List of Excluded Individuals or Entities (LEIE), and the GSA/SAM (System for Award Management) website prior to hiring and monthly there after to ensure that none have been excluded from participation in the program since the last search. (Alabama Medicaid Provider Manual, 7.3.1, January, 2019.)
II. Additional Alabama Exclusion Screening Requirements Arising from Provider Enrollment
Provider must identify all owners, officers, shareholders of greater than 5%, agents, directors and managing employees and, for each, disclose whether than have ever been excluded, debarred, or sanctioned from any state or federal program. (Alabama Provider Disclosure Form, amended July 2018.)
III. Excluded Parties are Banned From All Participation in Alabama Medicaid
Excluded entities are banned from participating in Medicaid and the program will not pay for any item or service furnished by or at the medical direction of an excluded party. The payment prohibition extends to services that are not directly billable such as nursing care in ahospital or nursing home; indirect services that like preparingsurgical trays or inputting prescription information; and administrative, IT or management duties. The ban also applies if the excluded party provided the item or service only partly or indirectly, and it extends toall methods of reimbursement (whether bundled, fee-for-service, or other). (Alabama Administrative Code, Rule No. 560-X-4-.04;Alabama Medicaid Provider Manual, 7.3.1;Section 1903(i)(2) of the Social Security Act; and 42 CFR sections 1001.1901(b)) and 1002.211)
IV. Who Gets Excluded? Why are Exclusions Imposed?
Alabama can excluded its providers for its Medicaid program for a variety of reasons. However, the most common reasons are:
- Felony Convictions
- Have been found guilty of Healthcare Fraud
- Patient Abuse
Adverse actions by licensing boards such as the Board of Nursing or the Medical Board
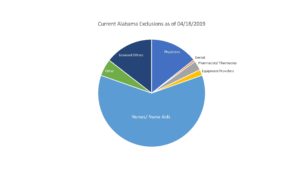
To understand what types of providers and employees are excluded the most, look at our chart below.
V. Liability From Employing or Contracting with Excluded Parties
All payments for services or items provided directly or indirectly by an excluded entity are potential overpayments. In addition, civil monetary penalties may be imposed against Medicaid providers and managed care entities (MCEs) who employ or enter into contracts with excluded individuals or entities to provide items or services to Medicaid recipients. (Section 1128A (a) (6) of the Act; and 42 CFR section 1003.102(a) (2)). Alabama Medicaid Provider Manual. Section 7.3.1).
Final Thoughts
In almost all instances, exclusions result from fraud, patient abuse or neglect, and/or drug related offenses, so employing or contracting with excluded parities pose direct risks to your practice or organization in addition to the potential legal consequences that can result from governmental oversight. Thus, Exclusion Screening provides an additional (and cost-effective) layer of risk reduction. So let us help you Protect Your Patients; Protect Your Practice; and Protect Yourself — call us at 1-800-294-0952 or fill out the form below to find out how Exclusion Screening can help you with monthly screening of the Alabama exclusion list and all other exclusion lists.
Article written by Paul Weidenfeld.
This document is for informational purposes only and not for the purpose of providing legal advice. You should contact your attorney to obtain advice with respect to any particular issue or problem.