The failure to report excludable offenses by state Medicaid offices and licensing boards is a longstanding issue for the OIG. Recent OIG audits and reports have confirmed these state failures to report. For example, an OIG study released in August found that over 12% of terminated providers were able to continue participating in other state Medicaid programs because states were not sharing terminated provider information. In addition, two recent Medicaid Fraud Control Unit (MFCU) audits discovered that they routinely failed to timely report conviction information to the OIG and sometimes did not report them at all.[1] Reporting failures lead to gaps in the OIG Exclusion List (LEIE) because the OIG cannot exclude an individual if the OIG is never informed of the state’s conviction, termination, or suspension of providers. Such failures to report are important because the information that would have been reported can lead to exclusion violations, which are listed on the LEIE. But, state compliance failures are not the only cause of gaps in OIG and State exclusion lists – as we discuss, no matter who is at fault, the provider may pay for anyone’s mistake.
I. The OIG Exclusion List Has Limited Search Capabilities
One important reason providers should not rely on screening only the LEIE is that its search function is extremely narrow. If an excluded individual uses a different name, such as a middle or maiden name, an LEIE search using the person’s first and last names may not produce any results.[2] For example, J. A.[3] was excluded from participation on Georgia’s state exclusion list in August 2015. However, a search for “J.A.” on the LEIE currently produces zero results.
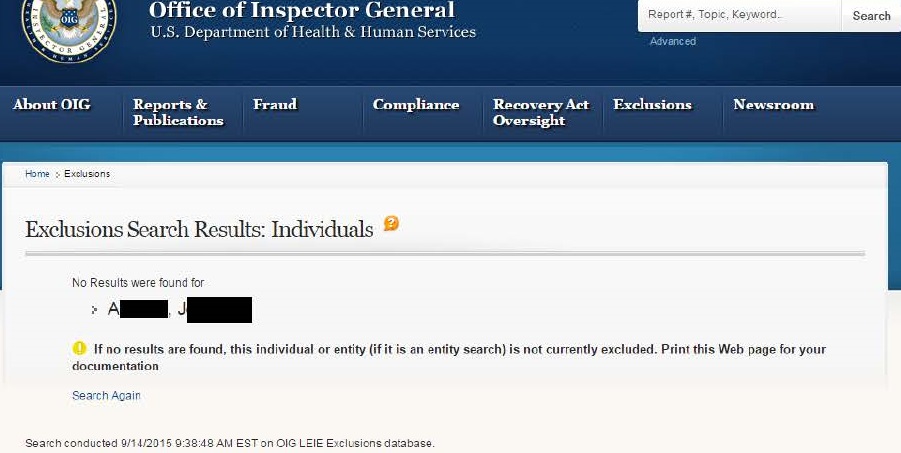
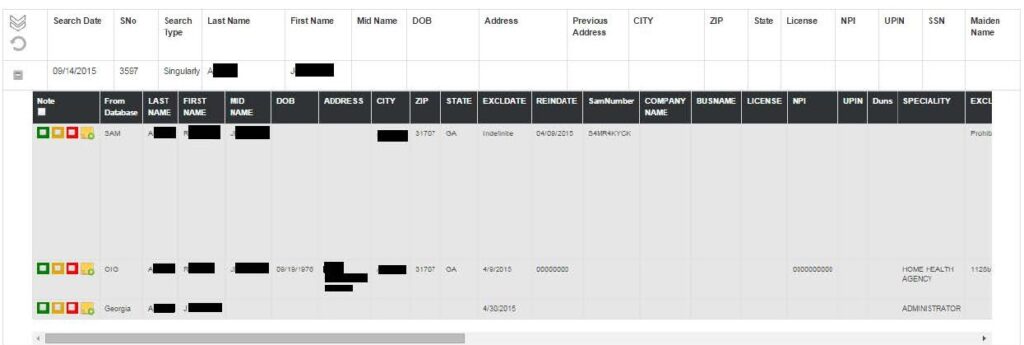
Conversely, when we searched J.A. on SAFERTM, our proprietary exclusion database, we not only found a match on the Georgia list (“J.A.”), but we also found a match on the LEIE and SAM databases for “R.J.A.”. Interestingly, “J.A.” has the same middle and last name as “R.J.A.,” they are both Georgia residents, and they were both excluded from participation in April 2015. Like many states, the identifying information on Georgia’s list is sparse. Nevertheless, R.J.A. and J.A. are likely the same person, which a provider would have missed if he only searched the LEIE for J.A.
Reported Cases May Not Be Picked Up by OIG
Florida’s Agency for Health Care Administration publishes monthly press releases that identify persons terminated from participation in Florida Medicaid. It expressly states that the exclusion information was “reported to the federal government for placement on the federal exclusion list,” and named providers appear on Florida’s Excluded Provider List. When we conducted a SAFERTM search for G.B., who was listed on the April 2015 memo as “terminated from participation,” the only two “hits” were from Florida’s state exclusion list.
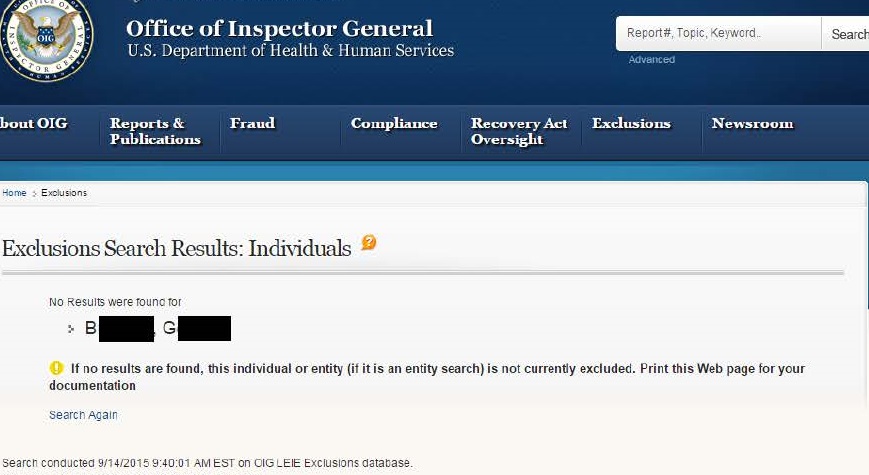
One possible explanation for why G.B. fails to show up on the LEIE could be the administrative process of OIG actually reviewing the reason for the termination and then formally excluding G.B. Nevertheless, a provider who only screens the LEIE and employs or is considering employing G.B. would miss this exclusion.
II. OIG Just Misses Some Cases
K.B., a Registered Nurse (RN) with multistate licensure privileges, was placed on probation for substance abuse in February 2005. After testing positive for morphine, Iowa revoked her license and several other states revoked her multistate privileges. While the revocations were reported, the licensure revocation only resulted in K.B.’s exclusion from participation by California and the GSA-SAM in 2010. K.B. is not listed on the LEIE. This means that K.B. is unable to participate in any other state Medicaid program because under the ACA 6501, if you are terminated for cause from participation in one state, then you are terminated in all states, and K.B. is barred from contracting with the federal government. However, if a provider only screened the LEIE he would be completely unaware and could potentially face very hefty fines.
III. What This Means
Clearly, some information is getting lost or mixed up in the reporting pipeline between state Medicaid offices, MFCUs, and the OIG, and the lesson for providers is that merely screening the LEIE is not enough. The examples above demonstrate that human error, narrow search functions, and simply missed information all play a role in the gaps that exist between publications on state exclusion lists and the LEIE.
State Medicaid offices are responsible for compiling and reporting information about excluded providers. However, as demonstrated by the “J.A.” case, the probable human error of transposing names combined with the LEIE’s limited search capabilities could result in a provider employing an excluded person, even though he was properly screened against the LEIE. To avoid this, providers should screen against the LEIE, the GSA-SAM, and all available state lists monthly. Practices should also ensure they use wide search parameters (alternate spellings, full names, maiden names, etc.) when conducting searches or they should select a vendor, like Exclusion Screening, LLC, with a system designed to anticipate these issues.
Notwithstanding name discrepancies, some information just does not make it to the LEIE. As the “G.B.” example reveals, a practice may face considerable monetary fines because it failed to screen the Florida exclusion list and relied solely on the LEIE for exclusion information, and the OIG failed to add G.B.’s name to the LEIE. Similarly, a provider who considered employing “K.B.” would be totally unaware that she was excluded from participation unless the provider screened the GSA-SAM and/or the California exclusion list. Remember that ACA section 6501 states that when an individual or contractor is excluded in one state, he or she is excluded in all states. When a provider misses such state exclusion information, he or she could be liable for CMPs of $10,000 for each claim provided directly or indirectly by the excluded individual, an assessment of up to three times the total amount paid by the government, and potential false claims liability. Relying on the LEIE’s exclusion information without checking all other available state exclusion lists is a substantial monetary risk for a practice to take.
Are you taking the necessary precautions to ensure you are not working with an excluded entity? We know it can be difficult to screen every Federal and State exclusion list. Call Exclusion Screening at 1-800-294-0952 or fill out the form below to hear about our cost-effective solution and for a free quote and assessment of your needs.
[1] MFCUs are supposed to send a referral letter to the OIG within 30 days of sentencing for the purpose of alerting the OIG about providers excluded from state programs, but the OIG found that in some cases this exclusion information was not referred to the OIG for over 100 days.
[2] We have even found that hyphenated names frustrate LEIE searches even where the actual names are used!
[3] Full names have been redacted for privacy.